Disclaimer: Any views expressed by individuals and organisations are their own and do not in any way represent the views of The Heritage Portal. If you find any mistakes or historical inaccuracies, please contact the editor.
What we see now happening worldwide with the Coronavirus is not new to Potchefstroom. Pandemics have passed through the city in the past. Three of them stand out.
Although the Rinderpest did not kill humans, except those who ate the flesh of infected animals, it caused wide-spread devastation in the country. This lead to desperate attempts at containing the spread and aid to impoverished farmers afterwards. Likewise the “Spanish” influenza, or flu for short, of 1918/9 devastated South Africa. In Potchefstroom it caused the deaths of many. In 2003 Potchefstroom also had to prepare for a disaster when three students died of meningitis in the city. As with the current Coronavirus crisis public places were closed as a precautionary measure and sports and other events were cancelled.
The story below was first published on my blog: lenniegouws.co.za, which focuses on the history of Potchefstroom.
Rinderpest
The devastation caused by a highly infectious disease was seen in 1896/7 with the outbreak of Rinderpest.
It is estimated that 2,5 million animals perished from the disease, both domesticated and wild animals. Rinderpest affected all ruminating animals with cleft hoofs, except small game.
In 1975 a former transport-rider told his memories to Prof JH Coetzee of the Potchefstroom University for Christian Higher Education and it was published in the second book in a series on the Groot Marico, called: Transportry, Runderpes en Poskoetse. He was CF Gronum.
The word Rinderpest is derived from German meaning cattle plague.
According to Gronum the Rinderpest was introduced to Africa in the port of Beira, Mozambique at the end of 1895 where bulls carrying the disease were disembarked. The bulls were imported from Europe by Cecil John Rhodes. It spread quickly westwards and by 1896 it had reached Salisbury (currently Harare in Zimbabwe). It killed all animals. Transport-riders travelled as far as they could go, expecting the disease to hit anytime.
One group of 30 wagons each drawn by 18 oxen, outspanned one evening and the disease hit the next day. Within eight days only two of the 540 oxen were alive. An infected animal would start to discharge fluids from their eyes and nose, standing with their backs bowed. Their faeces were completely black and they would drink copious amounts of water. Some would die at the water, some would walk back to their yokes and die there.
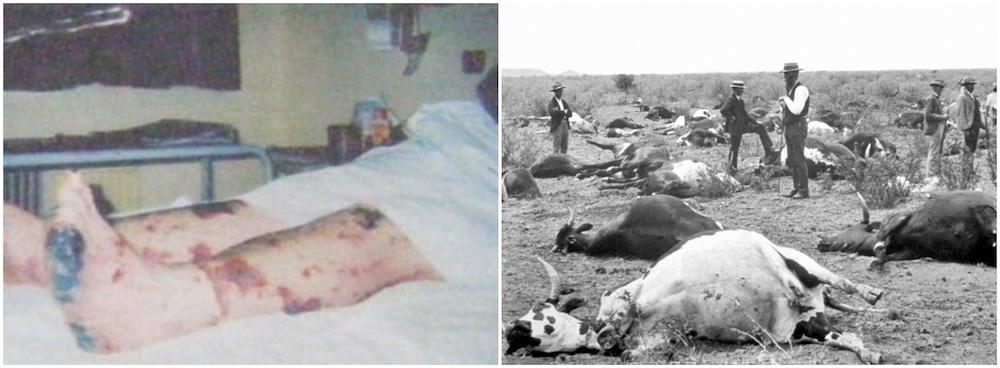
Cows dead from Rinderpest 1896 (via Wikipedia)
All our animals were dead
One transport-rider remarked: “All our animals were dead, oxen we have known for years, we trained them and we lived by their strength. All we could do was to leave our wagons with loads to the value of thousands of pounds behind and walk home.” They started the long walk home only with what they could carry. The smell of rotting carcasses was horrific. Vultures were everywhere but did not touch the rotting carcasses. Local tribespeople who ate the contaminated meat died as quickly as the oxen themselves.
The transport-riders on foot passed other wagons and had to help themselves to tin food on those wagons to survive. They also saw wagons that were plundered and burned.
The government tried to contain the disease by putting up wire fences, which was to no avail. The fence was to stretch from Rustenburg, through Groot Marico in the direction of Jagersfontein. Poles were planted, but before the fence could be erected the disease passed. The lone poles stood in the fields for many years afterwards.
Some farmers tried to inoculate their animals, only to give them the disease after which they anyway died within days. The government then ordered all living oxen to be shot. Farmers were to dig a huge hole, bring all their cattle to this hole where policemen shot the animals and the carcasses were buried. It was a horrific experience.
One farmer started to inject healthy animals with the puss oozing from an infected animal. This seemed to inoculate the animal.
Sir Arnold Theiler (1867-1936), regarded as the father of veterinary science in South Africa, visited the farmer, added glycerine to the mix and animals were thus inoculated.
In Potchefstroom the first case of the disease was on the farm Ratsegaaiskraal, owned by Abraham Kotzé. Contaminated meat was inadvertently brought to the farm by a sangoma. This was recorded by magistrate CH Douthwaite of Potchefstroom in a report to the government.
Afterwards a programme was launched by the government of the ZAR to aid impoverished farmers. In August 1897 an amount of £2 000 was made available to the magistrate of Potchefstroom. Destitute farmers were employed to repair roads and bridges and every Saturday afternoon £200 was paid out. This was by far not enough and in July 1898 a further £3 000 was made available to the magistrate of Potchefstroom. A further £750 was authorised with which the work was to be completed.
Price of an ox escalated nine times
Oxen that could be bought for £5 per animal before the Rinderpest, cost £45 afterwards. Slowly transport-riders started out again, some with donkeys drawing their wagons. If they found an abandoned wagon next to the road which was in a better condition than their own, they would load their freight on the better wagon and leave the other one behind. Nobody seemed to mind.
Ironically the Rinderpest also caused the demise of a prized herd of eland owned by Cecil John Rhodes in the Cape.
Dr Robert Koch, a German bacteriologist, developed a vaccine made from the gall of animals who died on the fifth or sixth day after being infected. Eventually 2,5 million animals were inoculated.
The disease again made its appearance in 1903, but not with the devastating results of the late 1890s.
In 2011 the World Organisation on Animal Health declared that the disease was eradicated, but in May 2012 it was said that the disease appeared again in Tanzania.
1918 flu
Sources vary about the origin of the Spanish flu of 1918/9, with the three main ones being Northern China, a British army base in France and Kansas in the United States. It was first observed and recorded in Kansas in January 1918 and it is estimated that it caused the deaths of 50 to 100 million people worldwide. It is argued that the malnourished and exhausted soldiers fighting in the First World War may have aided the spread of the disease. More soldiers died of the flu than on the battlefield in four years of fighting.
It was called the Spanish flu because Spain, which was not at war, allowed newspapers to openly report on the flu. Due to the war news reports that could damage morale were prohibited in countries at war.
A patient would initially show flu-like symptoms. More severe symptoms were that people would bleed not only from their noses and mouths but also from their eyes and ears. People would turn dark blue from lack of oxygen. An American doctor said that some patients’ skins were so dark that they could not tell white soldiers from African-American soldiers. The Potchefstroom Herald said that patients would eventually drown from fluids in their lungs.
According to South African History Online its arrival in South Africa is linked to two ships, the Jaroslav and the Veronej, who arrived in Cape Town on 13 and 18 September 1918, carrying members of the South African Native Labour Contingent (SANLC) on board. The ship docked in Sierra Leone before coming to Cape Town, a city associated with severe outbreaks of the flu.
The spread of the flu hit South Africa from two points of entry, the first starting in Durban and moving to the Witwatersrand. The second started in Cape Town, then affected the Free State and the Western-Transvaal. A second wave from Cape Town travelled through the Eastern Cape and the Transkei.
It is estimated that 500 000 South Africans died, the fifth hardest hit country in the world.
The Potchefstroom Herald reported extensively on all matters regarding the flu from the first mention of cases until after it seemed that new cases seemed to decrease. First reports appeared on 8 October 1918, when it was said that most doctors saw as many as 60 cases per day.
The town council took control and appointed nurses for each municipal ward, who had to visit houses and tend to the sick. The hospital, built in 1914, was overrun with patients and tents were erected to accommodate them.
The advertisement requesting help was published on 15 October 1918 in the Potchefstroom Herald.
The town council voted to allocate £500 for preventative measures. This included the setting up of dispensaries in the Location, Southern Burger Rights and Northern Burger Rights and the town. It was recommended that the Chamber of Commerce and commercial community generally close their businesses at an early hour in order that their assistants may be in fresh air as much as possible. It was thought that exposure to fresh air would prevent and cure the disease.
Heart-breaking stories are told: In one instance 33 very ill people were found sheltering in a little building.
In another case a man, whose wife had succumbed a week before, was found lying in an advanced stage of pneumonia, with a little boy lying in the same bed, and five other children – all girls – lying on the floor of the living room, without attendance of any sort.
“Particularly distressing is the case of Mrs Hudson, who died during the weekend. In this household are six motherless bairns, including twin infants, only a fortnight old. Their father is fighting in Flanders.”
At the height of the outbreak the Herald expressed its shock with a wife who wrote a letter to a barber requesting him to come and shave her husband. “He is ill with Spanish influenza and can’t get out.”
The Herald published these appeals on 18 October 1918.
On 22 October the Herald reported: “The sights – and smells – that have met the voluntary workers in the last few days are simply appalling – poverty, starvation and misery; children crowded into shanties where their elders are lying stricken with fever and pneumonia.”
At the time it is estimated that a 1 000 people were ill. It is difficult to say what percentage of the population it was. In 1911 there were 64 364 people living in the town and district.
Two well-known residents who passed away were Isaac Nathanson, owner of the North Bridge Mill and the acting district surgeon, Dr Roytowski. Dr P Roytowski (34) hailed from Poland and had been in Potchefstroom for only two years. Dr W Mortimer, who earlier moved to the Cape, visited Potchefstroom to sell his furniture, contracted the disease here and died.
As in the rest of the country the black and coloured population were hardest hit. A soup kitchen was established to supply food to stricken families and voluntary nurses tended to the sick.
By 5 November schools and bioscopes were open again and it seemed that life was slowly turning back to normal.
A second wave
A new wave of influenza hit the town in July 1919. On 6 July the first case was reported in the Herald.
The yearbook of the Potchefstroom University College (PUC) of 1919 stated: “Who could not remember the dark days of October 1918 when we had to carry one of our own to the grave? Who can forget last quarter when the flu claimed its numerous targets and we had to stand in front of an open grave twice on one day? Small wonder that we were shocked to our core.”
Elsewhere in the publication staff and the wives of lecturers of the PUC were thanked who took in ill students, far from their own families, into their houses to nurse them. The wives of Prof Kamp and Dr Los were thanked, as well as the housemaster of the hostel, Prof Ferdinand Postma.
The hostel of the Theological School was built in 1905 as part of the Theological School complex. It was later named after Prof Jan Lion-Cachet a former rector of the School. To this day theological students of the North-West University still live in the building. (NWU Archives and Museum)
Prof Ferdinand Postma (1879-1950) was housemaster of the hostel of the Theological School during the outbreak of the Spanish flu. He became rector of the newly formed Potchefstroom University College in 1921 and served in this capacity until his death. (NWU Archives and Museum)
Yellow clay and orange juice
Mrs Maria Kamp, wife of a lecturer at the PUC, Prof Jan Kamp, in her youth, received training at a sanatorium in Germany. She played a large role in the fight against the disease. The home of the Kamps were transformed into a semi-sanatorium with eventually 61 beds in every possible space in the house and in the yard. Even pergolas in the garden were covered in shade-netting to house patients! With her methods in naturopathy she cured an estimated 100 patients and no-one in her care died! The bodies of patients were smeared with a yellow clay that was taken out of the Mooi River just below the Potchefstroom Dam. The clay was first prepared before it was applied. Patients also had to drink copious amounts of orange juice.
By public demand and privately funded Mrs Kamp opened a sanatorium just outside Potchefstroom, called Sanitas. The Kamp family later moved there. Sanitas was situated just north of the Northbridge between the Mooi River and the Carletonville road. The northern border was the railway line.
Mrs Maria Kamp, wife of Prof Jan Kamp (1861-1924), was trained in naturopathy in Germany. Prof Kamp, who was educated to become a teacher in his native country, the Netherlands, came to South Africa in 1898 for health reasons. He was a lecturer at the Literary Department of the Theological School of the Reformed Church (predecessor of the PUC). The nursing methods of Mrs Kamp saved the lives all the patients in her care during the 1918/9 outbreak of Influenza. (NWU Museum and Archives)
One of the victims at the PUC was a student, Gert Hendrik van der Walt (20), who was described as “Lang Gert”(tall Gert), widely regarded as a friendly and vivacious person.
The registrar of the PUC, Rev WJ de Klerk, lost both his wife, Mrs Aletta Johanna De Klerk (36), who passed away on 21 August 1919 and a daughter, Lettie (11), who died six days later on 27 August.
After his shocking loss, he had eight more children to take care of on his own. A former housemaster of the hostel of the PUC, Piet van der Walt and his wife lost two foster daughters who died within nine days of each other in August 1919.
The registrar of the PUC, Rev WJ de Klerk, was left a widower with eight children when his wife, who was only 36 and one daughter, died. (NWU Museum and Archives)
On 22 August 1919 the Herald wrote: “While it is not possible to state accurately the number of cases in town and district, a moderate estimate, based on the scanty information at hand, places the total at 500”.
Worldwide it was estimated that 50 to 100 million people had died. If the death toll was to have been calculated today in terms of the percentage of the population 225-400 million would have died.
2003 – Meningitis brought city to a standstill
In early July 2003 a Potchefstroom student, who studied beauty therapy, died in the local Medi-Clinic. She was admitted to the High Care Unit with flu-like symptoms and died shortly afterwards. It was ascertained that she suffered from Neisseria meningitis, or meningococcal meningitis, a rare form of meningitis, which is highly contagious.
Three weeks later another student died of the same illness. This prompted an emergency meeting of medical professionals, including pathologists, specialist physicians, emergency room staff and the Department of Health. The latter subsequently issued a statement to create awareness.
A third student died within a week. The Potchefstroom Herald, on 25 July, reported extensively on all aspects of the situation.
The front page showed a photograph of a visually stressed mayor, Satish Roopa, his brother Mahesh Roopa and the director of health and environmental matters of the city council and Dr Theuns Oosthuizen, director in chief of Health Services in the North-West Province. An operational centre to monitor the situation was established in the council chambers of the city council.
Another report recaps all events since the death of the second student. Captions read: “How did students react”, “Residents swamped doctors, pharmacies”, “Van Bommel dies, more students are treated” (Mr Van Bommel was the second student who passed away), “Thousands receive medication” and “Minister of Health and WHO (World Health Organisation) help to combat meningitis”.
Photos of students wearing medical masks eerily remind of photos now seen and photos from 1918 Spanish flu outbreak.
The opinion was expressed that students might have contracted the disease in a club frequented by students and owners of these clubs decided to close their establishments for a few days as a voluntary attempt to alleviate the situation.
The Potchefstroom University decided to suspend all activities. The Intervarsity against the UOFS on 8 and 9 August in Bloemfontein, which was initially postponed, never took place. Over the 70 years the Intervarsity took place, it was a high point in the calendar. It was only cancelled seven times, one of the other times was due to World War II.
The positive side
Representatives of the WHO, who were in the city to assist, expressed their surprise at the number of diverse people who were able to act together in the crisis. “It is the first time we came across a mayor and community that are able to handle and manage such a situation. People have no qualms in offering their time.”
The editorial of the Herald of 1 August stated:
The people of Potchefstroom have showed what they are able to do with the managing of the outbreak of meningitis... The diversity of peoples out of different communities who worked together indicate a unity what crises like these requires.
By 8 August the Herald proclaimed: “Potch waits with bated breath.” Kiewiet Scheppel wrote: “The meningitis crisis seems to be something of the past. But the combined task teams can only relax when two incubation periods of the illness elapse on Monday 11 August.” Thereafter activities in the city and on the campus of the PU slowly got back to normal.
In spite of attempts to trace the origin of the outbreak, officials were unable to do so.
The funny side
In a more humoristic manner, two reporters of the Herald, Jaco Mostert and Marzahn Botha, combined forces to do a report on all the tall tales that floated around the campus.
One of the SMS’s said: “You are not in danger to contract meningitis, a brain is a determining factor. PUK Greetings, Theuns Eloff.” (Dr Eloff was the rector of the PU at the time.)
An unverified rumour under the students indicated that they should be on “the pill”. Some confused birth control medication with the prophylactic medication prescribed for meningitis. A pharmacist on the Bult, near the university, confirmed that they were swamped by students, wanting birth control medication!
A male student who one night became drunk, danced on a table and fell on his head, was convinced that he had the “symptoms”, but his doctor told him that he just suffers from a hangover and concussion.
One student was extremely upset when he found that all the clubs were closed. “What does one do when you can’t go to a club!?” The rector’s reaction: “what can you expect from students?”
The Alabama Student Company had a show in Vanderbijlpark during the time of the crisis, which could not be cancelled. When the curtain was raised the performers saw that the first few rows of the otherwise packed hall was empty, creating a “safe” space.
By 15 August the crisis was a thing of the past and the operations of the task force suspended after giving certificates to acknowledge the work of everybody involved in the crisis. At this event the mayor said: “We were in a war, we all wore the same uniform and we set aside our differences to win the war”.
The aftermath
All together 93 patients showing symptoms of meningitis were treated. Nearly 15 000 prophylactic tablets were distributed and only four persons, identified by health services, were inoculated against the disease. The estimated costs of the outbreak was R629 000.
In September 2003 a 19 year old barman, Trevor Harris, of a pub next to the N12 near Potchefstroom contracted meningitis, causing a new scare. A spokesperson of health services said that it was regarded as a single case, since Trevor worked in a public place next to an interprovincial route.
By January 2004 Trevor’s feet were still in bandages after four of his toes, two on each foot, were amputated and dead tissue was removed from his feet. The bacteria of the meningitis destroyed the small veins in his feet and legs and due to a lack of blood and tissue in his feet and legs was destroyed. The bandages had to stay on till February. It was expected that he would walk again.
Trevor Harris (19) contracted meningitis in September 2003. On 26 September 2003 this photo appeared in the Herald and clearly shows the devastation the illness caused and showed how his feet and legs looked shortly after he was admitted to the hospital.
About the author: Somewhere in her late teens Lennie realised that writing came easy to her and now, many decades later, she has written and co-written nine books on various aspects of the history of Potchefstroom. This is apart from various supplements and numerous articles, mostly published in the Potchefstroom Herald. Two of her books are available on amazon.com. One is a biography on Kenneth McArthur, Olympic gold medallist in the marathon of 1912. The other is an Afrikaans Christian novel. The supplement on the history of the Herald, at the time of its centenary in 2008, led to a Master’s degree in Communication Studies and one of the books, on NWU PUK Arts, led to a PhD in history. In the process of all this writing she has accumulated a large stash of information and photos on the history of Potchefstroom.
Sources:
- CF Gronum, Transportry, Runderpes en poskoetse (Potchefstroom, 1975).
- HG Schulze ed, Veritas Vincet Jubileumuitgawe (Potchefstroom, 1919).
- JP Kotze, Die Runderpes in die Transvaal en die onmiddellike gevolge daarvan, 1896-1899 (MA dissertation, Rand Afrikaans University), 1974.
- PF van der Schyff, Sages en legendes en ander lekker stories oor die PUK volume 1 (Potchefstroom, 2003).
- Potchefstroom Herald
- Potchefstroom Museum, Potchefstroom Cemetery – graves of the residents of Potchefstroom 1903-2010.
- South African History Online, 2019, Spanish Flu strikes South Africa. https://www.sahistory.org.za/dated-event/spanish-flu-strikes-south-africa, accessed 12 March 2020.
Comments will load below. If for any reason none appear click here for some troubleshooting tips. If you would like to post a comment and need instructions click here.







